Revenue cycle management, often called RCM, is the process healthcare providers use to manage the financial side of patient care. It starts before a patient walks into the practice and continues until the provider receives final payment from insurance companies or the patient.
In simple terms, revenue cycle management connects patient scheduling, insurance verification, medical coding, claim submission, payment posting, denial management, accounts receivable follow-up, and patient billing into one organized system.
This matters because healthcare providers in the U.S. do not get paid just because a service was delivered. Payment depends on accurate patient information, proper documentation, correct ICD-10, CPT, and HCPCS coding, clean claim submission, payer rules, HIPAA-compliant data handling, and timely follow-up.
For medical practices, clinics, hospitals, and specialty providers, strong RCM is not just a billing function. It is the foundation of predictable cash flow, fewer claim denials, faster reimbursement, and a better patient financial experience.
Quick Answer: What Is Revenue Cycle Management In Healthcare?
Revenue cycle management in healthcare is the complete process of managing the financial journey of patient care, from appointment scheduling and insurance verification to medical coding, claim submission, payment posting, denial management, and final collection.
In simple words, RCM helps healthcare providers get paid accurately and on time for the services they deliver. It connects the clinical side of care with the financial side of reimbursement.
A strong revenue cycle management process helps practices reduce claim denials, improve cash flow, prevent billing errors, stay compliant with payer and HIPAA requirements, and create a better patient billing experience.
What Is Revenue Cycle Management?
Revenue cycle management is the complete financial workflow that helps healthcare organizations capture, bill, collect, and reconcile payment for medical services. It includes every step that affects how revenue moves through a healthcare practice, from front-desk registration to final account resolution.
A strong RCM process answers three important questions:
- Is the patient covered for the service?
- Was the service documented and coded correctly?
- Was the provider paid accurately and on time?
When revenue cycle management works well, healthcare providers can reduce billing errors, avoid preventable denials, improve collections, and spend less time chasing payments. When it works poorly, even high-volume practices can face delayed cash flow, aging accounts receivable, underpayments, patient billing confusion, and revenue leakage.
That is why many practices treat RCM as a strategic business function, not only an administrative task.
RCM Meaning In Medical Billing
RCM stands for Revenue Cycle Management.
In medical billing, RCM means managing the full payment journey for healthcare services. Medical billing is one part of RCM, but RCM is broader. Billing usually focuses on creating claims, submitting them to payers, posting payments, and sending patient statements.
RCM includes those tasks, but it also covers eligibility verification, prior authorization, clinical documentation, coding accuracy, denial prevention, payer follow-up, reporting, compliance, and patient financial communication.
So, when someone asks, “What is RCM in healthcare?” the simplest answer is this:
RCM is the system that helps healthcare providers turn patient care into accurate claims, timely reimbursement, and final payment collection.
For practices that want expert support across this full process, Revenue Cycle Management Services can help manage the complete workflow from patient access to final reimbursement.
Revenue Cycle Management Vs Healthcare Billing Cycle
The healthcare billing cycle and revenue cycle management are closely connected, but they are not the same thing.
The healthcare billing cycle usually refers to the process of preparing, submitting, tracking, and collecting payment for medical claims. Revenue cycle management includes the billing cycle, but it starts earlier and goes deeper.
Medical billing often begins after the patient encounter has been documented. RCM begins before the patient visit, when the appointment is scheduled and insurance information is collected. That early work affects everything that happens later. If the practice records the wrong insurance ID, misses a prior authorization, or fails to verify benefits, the claim may be denied even if the provider delivered excellent care.
Revenue Cycle Management Vs Medical Billing
| Medical Billing | Revenue Cycle Management |
| Focuses mainly on claim creation, submission, and payment posting | Covers the full financial lifecycle of patient care |
| Usually starts after the patient visit is documented | Starts before the visit with scheduling, registration, and eligibility |
| Handles billing transactions | Manages front-end, mid-cycle, and back-end revenue processes |
| Helps submit and collect claims | Helps prevent denials, improve collections, and reduce revenue leakage |
| Mostly operational | Strategic, financial, operational, and compliance-focused |
Revenue cycle management also continues after the claim is submitted. It includes denial analysis, appeals, A/R follow-up, underpayment review, patient balance management, KPI tracking, and process improvement.
This is why RCM is more than “getting claims out the door.” It is a complete financial operating system for healthcare providers.
The Revenue Cycle Management Lifecycle
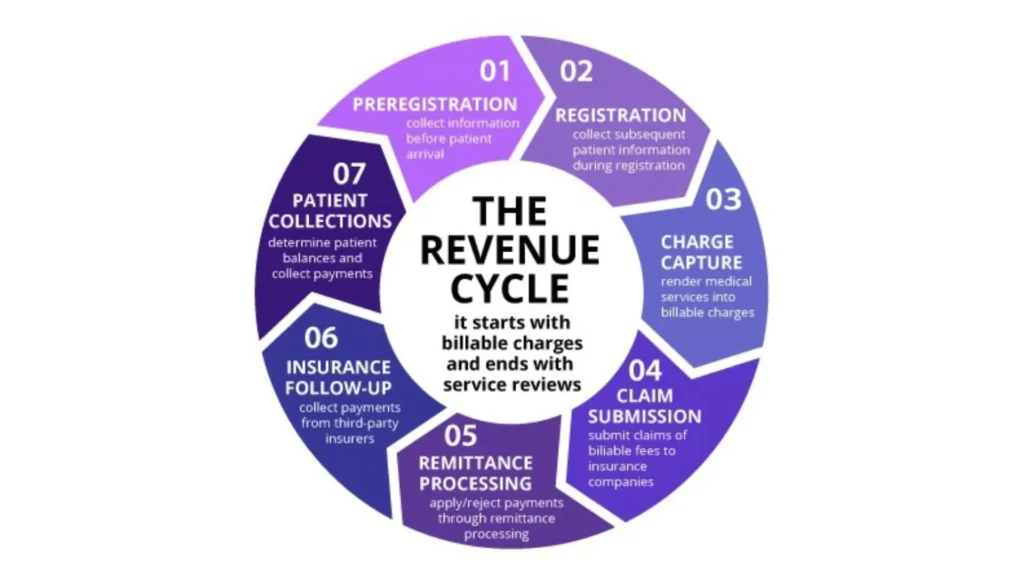
A complete RCM lifecycle can be divided into three major stages: front-end RCM, mid-cycle RCM, and back-end RCM. Each stage plays a direct role in whether the provider gets paid correctly and on time.
Main Stages Of The RCM Lifecycle
| RCM Stage | What Happens | Why It Matters |
| Front-End RCM | Scheduling, registration, eligibility verification, prior authorization | Prevents claim problems before the visit |
| Mid-Cycle RCM | Documentation, charge capture, ICD-10, CPT, and HCPCS coding | Turns clinical care into accurate billable claims |
| Back-End RCM | Claim submission, payment posting, denial management, A/R follow-up, patient billing | Helps providers collect payment and reduce revenue leakage |
Front-End RCM: Scheduling, Registration, And Eligibility
Front-end RCM starts when a patient schedules an appointment. This stage includes collecting patient demographics, insurance details, contact information, referral requirements, and financial responsibility information.
Accurate registration is critical because small errors can create major payment delays. A misspelled name, incorrect date of birth, inactive insurance policy, or missing subscriber information can cause claim rejection or denial.
Eligibility verification is also one of the most important parts of the healthcare billing cycle. Before the visit, the practice should confirm whether the patient’s insurance is active, what services are covered, whether a deductible applies, and whether prior authorization is required.
When front-end RCM is handled properly, the practice prevents problems before they become unpaid claims.
Mid-Cycle RCM: Documentation, Coding, And Charge Capture
Mid-cycle RCM begins after the provider delivers care. At this stage, the clinical encounter must be translated into billable services.
This depends on three things: complete provider documentation, accurate medical coding, and proper charge capture.
Medical coding connects the patient’s diagnosis, treatment, procedure, or service to standardized codes. In the U.S., this usually includes ICD-10-CM for diagnoses, CPT for procedures, and HCPCS for certain supplies, services, and Medicare-related billing.
If documentation is incomplete or the codes do not support the service billed, the claim may be denied, underpaid, or delayed. This is why medical coding is not just a technical task. It is one of the strongest links between clinical care and financial performance.
For providers that need help with claim creation, coding-related billing workflows, and payment follow-up, Medical Billing Services can support the billing cycle while reducing administrative pressure on internal staff.
Back-End RCM: Claims, Payments, Denials, And A/R
Back-end RCM begins once the claim is ready for submission. This stage includes claim scrubbing, clearinghouse submission, payer adjudication, payment posting, denial management, appeals, patient billing, and accounts receivable follow-up.
A clean claim is one that has the required patient, provider, service, diagnosis, and payer information needed for processing. Claim scrubbing helps identify missing or incorrect information before the claim reaches the payer.
After submission, the payer reviews the claim and decides whether to pay, deny, reject, or request more information. If the claim is paid, the payment must be posted correctly. If the claim is denied, the billing team must identify the reason, correct the issue, and appeal or resubmit when appropriate.
This is where many practices lose revenue. They submit claims, but do not follow up quickly enough. They receive partial payments, but do not review underpayments. They get denials, but do not track denial patterns. Over time, these gaps create revenue leakage.
How Claims Flow Through The U.S. Healthcare System
To understand revenue cycle management in healthcare, it helps to understand how a claim moves through the U.S. payment system.
The claim flow usually looks like this:
Patient visit → clinical documentation → medical coding → charge entry → claim creation → claim scrubbing → clearinghouse submission → payer adjudication → ERA/EOB → payment posting → patient balance → final collection.
For professional services, claims are often submitted electronically using the 837P format. CMS-1500 is commonly used as the standard paper claim form for professional claims.
This claim flow is important because every step depends on the step before it. If insurance verification is wrong, the claim may fail. If documentation is weak, the coding may not support the service. If coding is incorrect, the payer may deny or reduce payment. If payment posting is inaccurate, patient balances and reports may be wrong.
Strong RCM gives practices visibility across this entire journey. Instead of reacting to unpaid claims after months of delay, a good revenue cycle process identifies issues early and keeps claims moving.
Why Revenue Cycle Management Is Important For Healthcare Providers

Revenue cycle management is important because it directly affects the financial health of a healthcare organization. Providers need consistent reimbursement to pay staff, invest in technology, manage overhead, and continue delivering patient care.
A weak RCM process can lead to delayed payments, rising denial rates, poor patient billing communication, and growing accounts receivable. A strong RCM process helps providers improve cash flow, reduce administrative burden, and create a smoother financial experience for patients.
For private practices and medical groups, this matters even more. Many providers operate with limited staff. If the front desk, billing team, and clinical team are not aligned, revenue problems can appear quickly. Missed authorizations, coding errors, delayed claim follow-up, and unclear patient statements can all reduce collections.
RCM helps bring structure, accountability, and measurable performance to the business side of healthcare.
Common Revenue Cycle Management Challenges
Most RCM problems begin with small errors that grow into larger financial issues. A patient’s insurance was not verified. A prior authorization was missed. A diagnosis code did not support medical necessity. A claim was rejected by the clearinghouse. A denial was not appealed in time. A payer underpaid the allowed amount. A patient statement was confusing.
These issues are common, but they are not harmless. They increase staff workload, delay reimbursement, and make it harder for providers to understand their actual financial performance.
The most common RCM challenges include inaccurate patient registration, eligibility errors, missing referrals, prior authorization issues, incomplete clinical documentation, coding mistakes, claim rejections, payer denials, slow A/R follow-up, underpayments, and patient collection delays.
Common Causes Of Claim Denials In RCM
| Denial Cause | Where It Starts | How To Prevent It |
| Incorrect patient information | Registration | Verify demographics and insurance before the visit |
| Inactive insurance coverage | Eligibility | Check benefits before the appointment |
| Missing prior authorization | Front-end RCM | Confirm payer authorization rules before service |
| Coding errors | Mid-cycle RCM | Use accurate ICD-10, CPT, and HCPCS codes |
| Lack of medical necessity | Documentation and coding | Make sure documentation supports the billed service |
| Timely filing issues | Back-end RCM | Submit and follow up on claims quickly |
| Underpayments | Payment posting | Compare payer payment with contracted rates |
The best RCM teams do not only fix these issues after they happen. They study patterns and prevent them from repeating. For example, if a specific payer frequently denies claims for missing authorization, the practice can strengthen its pre-visit authorization process. If one service line has high coding-related denials, the team can review documentation and coding workflows.
That is how RCM moves from reactive billing to proactive revenue protection.
A Practical RCM Example
For example, a patient may arrive for a specialist visit with active insurance, but the payer may require prior authorization for that specific service. If the practice does not verify the authorization requirement before the visit, the claim can be denied weeks later even though the provider delivered medically necessary care.
This is why strong revenue cycle management is not only about submitting claims. It is about preventing avoidable errors before they delay reimbursement.
At Zeerak Care, this kind of front-end accuracy is a major focus because many back-end billing problems begin with missed eligibility checks, incomplete registration, or payer-specific requirements that were not verified early enough.
HIPAA, CMS, And ICD-10 In Revenue Cycle Management
Revenue cycle management handles sensitive patient, clinical, and financial data, so compliance is a major part of the process.
HIPAA plays a central role because billing teams handle protected health information, also known as PHI. Patient demographics, insurance details, diagnosis codes, treatment information, claim data, and payment records must be handled with privacy and security in mind.
CMS is also important because it provides rules, resources, and standards that affect Medicare billing, claim formats, coding, reimbursement, and provider compliance. CMS-related rules can influence how claims are prepared, submitted, corrected, and reimbursed.
ICD-10 matters because diagnosis coding helps explain why a service was medically necessary. If the diagnosis does not support the service billed, a payer may deny the claim. That is why accurate documentation and coding are essential for both compliance and reimbursement.
A strong RCM process protects revenue while also supporting privacy, accuracy, and payer-specific requirements.
Key Revenue Cycle Management Metrics To Track
A provider cannot improve what it does not measure. That is why RCM reporting should focus on the metrics that reveal claim quality, collection performance, payer behavior, and operational efficiency.
Important RCM KPIs
| RCM Metric | What It Shows | Why It Matters |
| Clean Claim Rate | Claims accepted without errors | Shows claim quality |
| Denial Rate | Claims denied by payers | Reveals coding, documentation, or eligibility issues |
| Days In A/R | Time taken to collect payment | Shows cash flow health |
| Net Collection Rate | Collectible revenue actually collected | Measures financial performance |
| First-Pass Resolution Rate | Claims paid on first submission | Shows billing efficiency |
| Cost To Collect | Cost of collecting revenue | Helps measure operational efficiency |
These metrics help practices identify where revenue is getting stuck. If clean claim rate is low, the issue may be registration, coding, documentation, or claim scrubbing. If days in A/R is high, the issue may be payer follow-up, denial management, or patient collections. If net collection rate is low, the practice may be losing money through write-offs, missed appeals, or underpayments.
Good reporting turns RCM into a management tool, not just a billing process.
The Role Of Automation And AI In Modern RCM
Revenue cycle management is becoming more technology-driven. Healthcare organizations are using automation and analytics to improve eligibility checks, claim scrubbing, coding review, denial prediction, payment posting, and reporting.
Automation can reduce repetitive manual work, but it does not replace human expertise. Payer rules, clinical documentation, coding accuracy, appeal strategy, and patient communication still require trained billing and RCM professionals.
For example, automation may help identify missing claim fields before submission, but an experienced billing specialist still needs to understand payer behavior, modifier usage, documentation gaps, and denial trends.
Modern RCM works best when technology and human expertise work together. Software can speed up repetitive tasks, while trained professionals make judgment-based decisions that protect revenue and compliance.
When Should A Practice Consider RCM Support?
A healthcare practice should consider professional RCM support when revenue problems become consistent instead of occasional.
Common signs include increasing denials, delayed reimbursements, aging A/R, overloaded billing staff, unclear financial reporting, frequent eligibility errors, coding-related rejections, patient billing complaints, and poor follow-up on unpaid claims.
Outsourced RCM support can be especially useful for solo providers, growing practices, multi-location groups, and specialty clinics that need stronger billing performance without increasing internal staffing costs.
A dedicated RCM partner can help manage eligibility verification, claims, payment posting, denial management, A/R follow-up, reporting, and patient billing workflows. This allows providers to focus more on care delivery while trained billing professionals manage the financial process.
Need Help Improving Your Revenue Cycle?
If your practice is dealing with delayed payments, rising denials, aging A/R, billing errors, or overloaded staff, professional RCM support can help you regain control of your revenue cycle.
Zeerak Care provides Revenue Cycle Management Services and Medical Billing Services for healthcare providers that want faster reimbursements, fewer denials, cleaner claims, and more predictable cash flow.
Our team supports the full billing workflow, from eligibility verification and claim submission to payment posting, denial management, A/R follow-up, and reporting, so your practice can focus more on patient care and less on paperwork.
Frequently Asked Questions About Revenue Cycle Management
What Is Revenue Cycle Management In Healthcare?
Revenue cycle management in healthcare is the process of managing payment for patient care from the first appointment to final collection. It includes scheduling, insurance verification, medical coding, claim submission, payment posting, denial management, A/R follow-up, and patient billing.
A strong RCM process helps healthcare providers reduce claim denials, improve cash flow, collect payments faster, and keep billing workflows organized.
What Does RCM Mean In Medical Billing?
RCM means Revenue Cycle Management. In medical billing, it refers to the full process of managing claims, payments, denials, patient balances, and collections for healthcare services.
Medical billing is part of RCM, but RCM is broader. It also includes front-end tasks like patient registration, eligibility verification, prior authorization, and compliance checks.
What Are The Main Steps In The Healthcare Revenue Cycle?
The main steps in the healthcare revenue cycle are patient scheduling, registration, insurance verification, prior authorization, clinical documentation, medical coding, claim submission, payer adjudication, payment posting, denial management, A/R follow-up, and patient billing.
Each step affects whether the provider gets paid accurately and on time. Errors early in the cycle often lead to claim denials or delayed reimbursement later.
Is Revenue Cycle Management The Same As Medical Billing?
No, revenue cycle management is not the same as medical billing. Medical billing focuses mainly on preparing claims, submitting them to payers, posting payments, and billing patients.
Revenue cycle management covers the full financial journey of patient care. It starts before the visit with scheduling and eligibility verification and continues through coding, claims, payment posting, denial management, A/R follow-up, and final collection.
Why Is Revenue Cycle Management Important For Healthcare Providers?
Revenue cycle management is important because it helps healthcare providers get paid accurately and on time. It reduces claim denials, improves cash flow, prevents billing errors, supports compliance, and gives practices better visibility into financial performance.
Without strong RCM, providers may face delayed reimbursements, aging accounts receivable, underpayments, patient billing issues, and lost revenue.
Conclusion
Revenue cycle management in healthcare is the complete process of managing payment for patient care, from appointment scheduling to final collection. It includes patient registration, eligibility verification, prior authorization, documentation, ICD-10 and CPT coding, claim submission, payer adjudication, payment posting, denial management, A/R follow-up, and patient billing.
The healthcare billing cycle is part of RCM, but RCM is bigger. It connects clinical, administrative, financial, and compliance workflows into one system that protects revenue and improves practice performance.
For U.S. healthcare providers, strong RCM is no longer optional. It is essential for reducing denials, improving cash flow, maintaining compliance, and creating a better patient financial experience.

